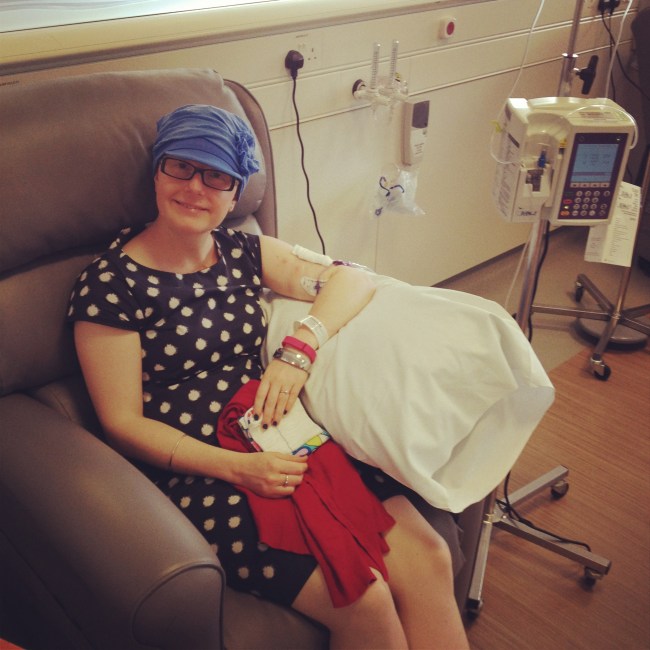
I have made a discovery. There are certain chemo side effects that don’t appear on factsheets and hospital consent forms. That’s not because they don’t exist, but because patients and consultants alike would have to endure a certain amount of embarrassment to reveal them.
They may not be groundbreaking and they’re certainly not on a scale of peripheral neuropathy or fatigue. But, I believe any side effect that brings about a physical change (embarrassing or otherwise) should be noted down so that a) we don’t all think we’re bonkers when it happens and b) we go into the entire process knowing there might be a few laughs along the way. So that’s what I’m about to do.
Before I begin, I think I should start with an apology, particularly to my loyal male readers. The following post may take you to places you’d really rather you didn’t know existed. There is about to be what one might call an element of oversharing. Trust me, it is not indulgent. It is medical. While I think it wrong to apologise for the route I am about to take, I can confirm that I will be containing it to a single blog post, so you don’t have to concern yourself with a repeat performance. Who knows? You might just find it funny.
I think it is fair to say that I’m not surprised certain side effects do not get a public airing. It takes me back to my hip surgery days. I remember waking up from the operation to find that my nether regions had been dyed a rather peculiar shade of purple. It was also a rather permanent type of dye, which meant I had to live with my alien-like hue for quite a while before the colour grew out. I had been prepared for the pain, the discomfort and the lack of weight bearing. I had not been prepared to laugh every time I took a shower.
Thoroughly amused by this turn of events, I raised the point at a focus group about patient care as a way of demonstrating that even the smallest of details are worth mentioning to help people deal with recovery. The patients all nodded in agreement as if reminding themselves of the discovery. The nurses laughed. And the surgeon? Well, he explained that they must have been out of the orange dye that week!
I am afraid to say it is this same region that has triggered my search for the secret chemo side effects everyone has, but no one dares to declare. Having never had a Brazilian wax, I was rather intrigued at the possibility of losing my hair on areas other than my head. But, I have to confess, it brought with it a rather unusual problem. Without being too crude, it seems the hair does help in a directional sense and its absence means you have to be vigilant (particularly if you have a tendency to crouch in public loos). Initially I thought it was just me, but having mentioned it to a few select ears (and done some rather entertaining Googling), it seems I am on to something! Now why didn’t the oncologist mention that when he was telling me about coping with hair loss! It may not warrant a whole fact booklet, but I think it deserves a paragraph. And, as an aside for women who trim regularly, I would urge you all to stop.
On the subject of hair loss, I think it strange that the advice tends to focus on the hair, eyelashes and the eyebrows. What about nose hair?! While losing the hair on your head is not to be recommended (unless you really do like the idea of trying out every short style you never dare attempt), it is manageable. Losing the hair in your nose, however, makes it look like you are dining on a diet of curries and hot foods.
And then there’s the growing back bit! While I am yet to enjoy this rather hairy experience, I am led to believe that the hair doesn’t always remember where it’s supposed to grow. I have heard of people shaving their big toes and not their armpits!
Why is it that everyone goes on about Epirubicin and the dreaded ‘pink pee’, but nobody talks or writes about Docetaxel and the ‘sweet pee’? I’d take coloured pee any day over something that smells like an overstocked sweetie store. For those of you about to embark on this taxing drug, you have been warned!
Even products designed to alleviate some of the more well-reported side effects, such as hot flushes, don’t offer up the full picture. I have been wearing the Ladycare magnet in my knickers for a week or so now in an attempt to get a good night of sleep. I am not sure it has reduced my sweats, but it has managed to attach me to everything from my dessert spoon to my door keys. Thankfully a kind friend warned me of this, so I wasn’t too alarmed when it happened for the first time. I don’t really like the idea of being joined at the hip with all metal items in the neighbourhood.
I should also mention that there are also positive side effects that I would have loved to have been told about upfront to balance things a bit. The consent form should say: ‘by signing up to this course of chemotherapy drugs please be advised that your skin will become silky smooth and soft.’
I should probably stop here before I lose all my followers. But, let me leave you with a few final thoughts. To all medical professionals out there, fear not the embarrassing, blush-inducing side effects! If we’re going to sign off a seven-page consent form, it is best to make it thorough! And to all cancer patients, please open up about those secret side effects (post here or make your oncologist blush).
Because, chances are, the person sitting next to you in the waiting room is experiencing them too.